Dry Eye Disease (DED), also known as Ocular Surface Disease (OSD) is a very complex condition that is chronic and progressive. More than 50% of those having the condition do not report symptoms, especially in the early stages. If dry eye disease is identified early, when mild, it is easier to treat, helping to slow the progression.
You may also download this document by clicking here.
The composition of the human tear layer is very complex with more than 500 unique proteins. For simplicity’s sake, let’s discuss the three main layers of the tears. There is the mucin layer which is the thinnest and helps to hold the tears on the cornea. It is important for the viscosity of the tears. The middle layer is the aqueous layer, which is the thickest layer, containing important nutrients for keeping your cornea healthy. The outer layer is the lipid or oily layer of the tears. The lipid layer is responsible for protecting the tear layer from evaporation, which is crucial in our high altitude and arid environment. This layer is produced by the meibomian glands, the openings of which line the lid margin just inside the lashes on the upper and lower lids.
There are two primary types of dry eye disease: evaporative and aqueous deficient. Evaporative DED is caused by Meibomian gland dysfunction and is present in over 80% of cases. Cases of purely aqueous deficient DED are fairly rare, occurring about 10% of the time. Many people have a combination of the two. Our testing protocol is designed to get to the base cause of the condition so that we can treat your DED more efficiently and effectively.
CAUSES OF DRY EYE DISEASE:
- Digital device use: screen time has increased exponentially and is probably the main reason the latest studies on dry eye show a significant increase in the condition in younger populations.
- Environmental factors: people tend to have dry eye symptoms when they are exposed to smoke, air pollution, high altitude, sunny, windy, cold or dry air conditions.
- Aging: tear flow normally decreases with age. About 75% of individuals over the age of 65 suffer from dry eye symptoms.
- Contact lens wear: contact lens wear can dramatically increase tear evaporation, causing dry eye discomfort.
- Hormonal changes in women: various hormonal changes associated with pregnancy, oral contraceptives and menopause can contribute to dry eye symptoms.
- Certain diseases: dry eyes are a problem with several diseases. Thyroid disease, arthritis, and lupus, are examples.
- Medications: the list of medications having dry eyes as a side effect is too extensive to list here. Check the package insert for any medications you are taking.
- Laser vision corrective surgeries and/or cataract surgery: following various ophthalmic surgical procedures patients can develop dry eye.
- Sjogren’s syndrome: an immune system disorder characterized by inflammation and dryness of the mouth, eyes and other mucous membranes. This disorder damages the lacrimal glands and affects tear production.

LIFESTYLE RECOMMENDATIONS
- 20/20 focusing breaks: every 20 minutes look 20 feet away for 20 seconds. This is recommended for patients who do a lot of reading or computer work. When we are doing concentrated activities we blink two to five times less frequently than normal, reducing tear production.
- Avoid direct air flow on your eyes: it is important to point all airflow including heating/AC vents, fans and defrosters away from your eyes. Avoid sitting under or sleeping with ceiling fans running.
- Remove makeup nightly: we all have glands in our eyelids that produce oil to help keep the moisture on our eyes. It’s important to clean the makeup off your eyes every night to make sure these glands can release the oil properly.
- Humidifier: keeping a humidifier in your house or next to your bed at night helps keep your eyes hydrated.
ADVANCED DIAGNOSTIC EQUIPMENT
KERATOGRAPH
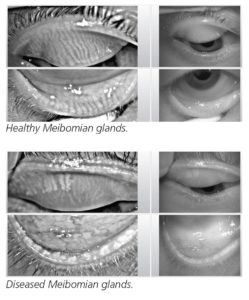
Examples of one component of the keratograph testing
The keratograph is one of several advanced diagnostic instruments and tests our doctors use to diagnose your dry eye disease accurately to help develop your individualized treatment plan.
The test results allow your doctor to objectively view the tear film and the health of your tear glands and to measure the tear evaporation rate. This procedure is FDA approved but not yet covered by your insurance. There will be a fee for this test in addition to any co-pay required by your medical insurance for the office visit. It is between you and your doctor to decide how often this testing is needed.
Fewer than 60% of dry eye patients are symptomatic. Early diagnosis makes it easier to treat this chronic condition and helps slow the progression.
DRY EYE SYMPTOM CHECKLIST:
- Blurry/fluctuating vision
- Red eyes
- Burning
- Itching
- Foreign body sensation, gritty, sandy feeling
- Light sensitivity
- Excessive tearing
- Pain or soreness in or around eyes
- Tired eyes
- Contact lens discomfort or intolerance
- Seasonal allergies
Ready to Schedule An Appointment?
The Highline Vision Center team is looking forward to seeing you soon. Our practice utilizes state-of-the-art technology to deliver personal and comprehensive eye care for your entire family.
